Benzodiazepines prescribed more in deprived areas, study confirms
In Clinical
Follow this topic
Bookmark
Record learning outcomes
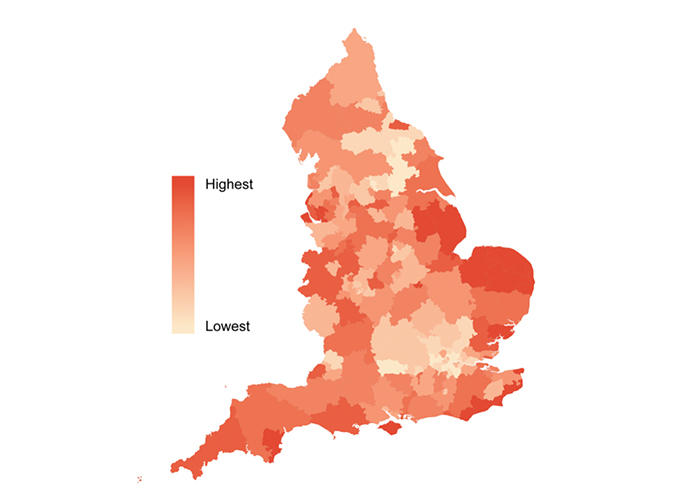
Benzodiazepines and Z-drugs are prescribed at higher rates to people living in deprived communities in England, new research from the University of Warwick has found.
The research team reviewed NHS Digital prescribing data from 2017 against NHS demographic information and a Public Health England deprivation metric that captures factors such as income, employment, education and housing.
They found that prescribing rates were 45 per cent higher in the most deprived practice populations compared to the least (288 prescriptions for benzodiazepines or Z-drugs per 1,000 patients versus 198).
The study also identified a “large geographical variation…with a tendency for higher prescribing rates to be seen in coastal region”. This “may be due to the older demographic in those regions,” the authors hypothesised.
The authors found that in total there were over 14 million prescriptions for benzodiazepines and Z-drugs in 2017.
Clinicians 'should consider alternatives'
Lead author Dr Saran Shantikumar from Warwick Medical School said: “The key result we found was there was an association between the amount of benzodiazepines prescribed in GP practices and the level of deprivation of people served by that practice.
“However, this is a very broad association. What we can’t tell from our analysis is which people within a given practice are getting those prescriptions. In fact, a recent report from Public Health England suggested that, if anything, individual patients from the least deprived practices were more likely to be prescribed these drugs. So we’re left with a conundrum: if fewer patients from the most deprived practices are being prescribed benzodiazepines, why do they tend to be prescribed higher volumes of them?
“One possibility is that the reasons for prescribing are systematically different between practices with high or low deprivation, and that those in more deprived practices are more likely to be given repeat prescriptions. Our finding that the relationship between deprivation and prescribing varied with different benzodiazepines lends some credence to that hypothesis.
“What clinicians can do is be aware that they may have patients who have been on these tablets for a long time and are potentially at risk, so it is worth actively thinking about whether a patient needs to continue taking those tablets or if there are alternative strategies.”
